Why Your Feet Might Be Making Your Prolapse Symptoms Worse
- Dr. Ashley Hocutt

- Mar 20
- 4 min read
Updated: Mar 23
When you think about pelvic floor symptoms like leaking urine or that heavy, pressure feeling in your pelvis, your feet are probably the last place you’d look.
But they matter—a lot.
Because your pelvic floor doesn’t work in isolation. It’s part of a full-body system that starts at the ground and moves up. And if your feet aren’t moving well, your pelvic floor often ends up picking up the slack.
Let’s Talk About Your Arch (Because It’s Not What You Think)
There’s a lot of focus on having a “strong arch,” which often turns into trying to hold the foot up or keep it from flattening.
But your arch isn’t meant to be rigid.
It’s meant to move.
When you walk, run, or even shift your weight, your foot should gently give into the ground and then rebound as you push off. That’s how your body absorbs and transfers force efficiently.
But here’s where people get tripped up—we don’t just want movement, we want control through that movement.
Because a foot that stays stiff isn’t helpful… but a foot that collapses without control isn’t either.
The Midfoot Is Where This Really Matters
This is the part that often gets overlooked.
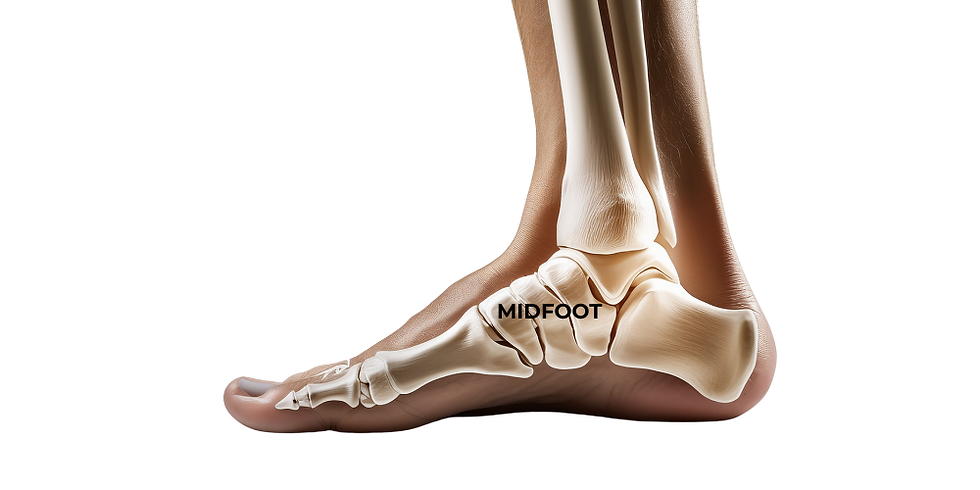
Your midfoot is designed to adapt. As you load into your foot, it should allow a small, controlled amount of flattening (pronation). That motion allows your shin and thigh bones to rotate, which then allows your pelvis to move.
And that pelvic movement? That’s what your pelvic floor depends on.
Without that natural rotation, the pelvis gets a bit more stuck.
And when that happens, your pelvic floor can’t get that subtle lift and recoil it’s designed for. Instead, it can stay more loaded or dropped, rather than springing back up to support you.
What I See Most Often
In the clinic, it’s usually one of two patterns.
Some people have a more rigid arch and midfoot, where the foot just doesn’t move much.
This isn’t usually intentional. It often develops over time—from things like a past ankle sprain, wearing shoes that don’t allow the foot to spread and adapt, or even gripping the toes for support. That constant tension can build through the plantar fascia and eventually into the midfoot itself.
So instead of the foot naturally yielding and rebounding, everything stays a bit more stiff—and the force from walking or movement has fewer places to go, so it travels up into the pelvis.
Others have the opposite pattern, where the foot drops quickly into pronation without much control. There’s movement, but not enough support to manage it.
Different patterns, same problem: the body loses its ability to smoothly absorb and transfer force.
What This Can Look Like in Real Life
I had a client who came in with prolapse symptoms specifically when running—leaking and a feeling of pressure that would show up pretty quickly.
We started where most people do: working on her core, breath, and pelvic floor.
And it helped—her symptoms improved by about 80%.
But something still wasn’t fully clicking.
When we looked further down the chain, her right foot told the rest of the story.
She had a history of an old ankle sprain, and her midfoot was stuck in a more supinated position, meaning she was loading more through the outside of her foot.
So even though her pelvic floor was stronger and more coordinated, the system underneath it wasn’t giving her what she needed.
We worked on restoring mobility in her foot, then built control in that new range—connecting it back up through her hip and pelvis.
And that’s when things really changed.
She was able to return to running leak-free for the first time in years.
So What Does This Have to Do With Leaking or Pressure?
Your pelvic floor is meant to act more like a trampoline than a tight grip.
It should lengthen as you load into it, then recoil to provide support.
But that only works if the system underneath it is doing its job.
If your foot is too rigid, your pelvis can’t rotate easily, and your pelvic floor loses its ability to lengthen and absorb pressure.
If your foot lacks control, your system becomes less stable, and your pelvic floor has to work harder to keep up.
Either way, this can show up as leaking with movement, that heavy or dragging sensation, or a feeling like things just aren’t being supported the way they should be.
It’s Not About Forcing a Fix
This isn’t about gripping your foot or trying to “hold your arch up.”
And it’s not about letting your foot completely relax and collapse either.
It’s about finding that middle ground where your foot can move, adapt, and still feel supported.
Because when your foot does that well, everything above it has a better chance to do its job too.
Your pelvis can rotate.Your body can absorb force.Your pelvic floor can respond instead of brace.
The Bigger Picture
If you’ve been doing all the pelvic floor exercises and still noticing symptoms, this might be the missing piece.
Your pelvic floor doesn’t just need strength—it needs coordination with the rest of your body. And that starts at the ground.
The Bottom Line
If you’re dealing with prolapse symptoms like leaking or pelvic pressure, your feet might be part of the story.
Not because they’re weak—but because they may not be moving, or controlling movement, the way they need to.
When you restore that balance, your body becomes a lot more supportive from the ground up.
Ready to Stop Guessing?
If this is resonating and you’re dealing with leaking, pressure, or prolapse symptoms, you don’t have to keep guessing what your body needs.
A pelvic PT evaluation is a chance to look at the full picture—how your feet, pelvis, and pelvic floor are working together—so you can feel more supported with every step.
.png)


Comments